Managing the risk of urban epidemics: The case of Ebola
The Ebola outbreak in the Democratic Republic of Congo (DRC) is one of the first urban Ebola outbreaks, specifically in Mbandaka, a city of over one million residents. This outbreak began in the rural town of Bikoro before spreading, and since April 2018, has resulted in at least 27 deaths and 58 suspected cases in total. One death and four cases have occurred in the city. In response, the World Health Organization (WHO) will send over 15,000 doses of the experimental Ebola vaccines to the country, as well as safe burial body bags to prevent exposure through the spread of bodily fluids during funerals. Merck, the vaccine’s developer, is providing the medication at no charge while GAVI, the Vaccine Alliance – a global public-private health partnership body – has provided $1 million to support health workers.
Vaccine delivery is logistically and operationally challenging. The outbreak began in Bikoro, which lacks basic infrastructure such as electricity and telecommunications; the vaccine requires being stored between -76 and -112 degrees Fahrenheit. The vaccines are being transported in special containers that can maintain that temperature range for six days and portable power generators are being brought in for additional energy.
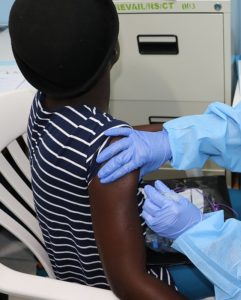
Local health officials have also taken steps to mitigate the risk of Ebola spreading; they have increased population tracing and identified 432 potentially exposed individuals. The early warning of cases in rural areas before appearing in urban areas provided emergency operations time to prepare. They are strategically inoculating the highest risk individuals, including medical workers and individuals that have had direct contact with infected patients, in order to create “rings” that act as buffers to further infection. The ultimate goal is to contain and treat the disease before it spreads to other population centers such as Kinasha, the capital of the DRC that contains over ten million residents.
Although this Ebola outbreak has been contained, this example shows the challenges that exist in managing global health care risks, ranging from poor infrastructure in vulnerable areas to the difficulty of containment in an increasingly interconnected world. The John Hopkins Center for Health Security simulated the impact of a global outbreak that spreads primarily via coughing, similar to a pandemic influenza, and does not have any antivirals or vaccines. This simulation involved a bipartisan group of current and former government officials simulating different executive roles. The simulation confronted them to with challenging decisions such as whether to impose travel bans, how to deploy the military, which groups should be prioritized in vaccine distribution, etc. The scenario ultimately escalated with the failure to develop a vaccine in 20 months resulting in the virus spreading through large cities, causing cascading effects such as health-care system collapses, market crashes, the incapacitation of significant portions of the US government, and over 150 million deaths.
The lessons learned from simulations and real world outbreaks demonstrate that the global healthcare has improved from past experiences, but requires greater coordination and investment to create a more resilient global healthcare system.
Further Sources and Reading:
- This mock pandemic killed 150 million people. Next time it might not be a drill. – Washington Post
- New Ebola vaccine faces enormous obstacles in crucial test for Congo outbreak – Washington Post
- More regions to be vaccinated, experimental drugs to be tried in Congo Ebola outbreak – CNN
- Congo warns of ‘new phase’ in Ebola outbreak after first urban case – Reuters
- The First Urban Case of Ebola in the Congo Is a ‘Game Changer’ – The Atlantic
- Factbox-As Congo Faces First Urban Ebola Outbreak, Experimental Vaccine Deployed – New York Times
